I Was Duped




Brent was a family man, everything he did was for our family.
“He was one of those people that it was just hard not to like him.”
This is my story about my husband Brent. He was overall a healthy active 34-year-old. We had four children ages 17, 13, 11, and 7. We have been together since 2007, and in 2009 we got married. Brent was a family man, everything he did was for our family. He did everything he could to make sure we were happy and had everything we needed. He never thought about himself. He would do anything for anyone. One of his favorite things to do was to coach our children’s little league football and baseball teams. He was one of those people that it was just hard not to like him. He was one of a kind.
Brent started having mild symptoms on October 18th. They were the kind of symptoms that he was used to considering he did have sinus issues from time to time. It wasn’t until the night of October 20th that he began to have more complex symptoms such as fever, body aches, and diarrhea. On the 22nd I went and got him a home Covid test. Brent took the test which confirmed that he had Covid. He then isolated himself in our bedroom to prevent us from getting it (Which none of us ever got). After the first few days of having the symptoms above, he began saying that he felt like he was getting better. Around 4:45 am on October 27 Brent called me (he was still isolating himself in the bedroom) and stated that he needed to go to the ER. I knew this was serious because he has never said those words in all the years, we have been together.
He was checked in at Tiffin Mercy Hospital on October 27 at 5:33 am according to his records. At first, I wasn’t allowed to come in with him, so I left and went home. I was at home approximately 20 minutes when I received a phone call from a woman at Mercy stating that I could come sit with my husband in his room. I left our home immediately and was there within 15 minutes. I’m not sure exactly what all took place before I got there, but he was sitting up in bed with a BiPAP oxygen mask on. It was hard for him to talk, but I do know that he just got back from doing a cat scan. He also complained of pain/numbness in his left leg. They didn’t know what was wrong with his leg, but they said he had Covid pneumonia. Not too long after I got there a doctor/nurse informed us that he was going to be transferred to Saint Vincent’s (Mercy) in Toledo, Ohio by life flight. We were also informed that they wanted to intubate him since he was being life-flighted. Of course, we had our concerns and didn’t want him to be on the ventilator. She validated our concerns and told us that the life flight crew might not require him to be intubated. So, we stated that we wanted to wait till life flight got there to see if he really had to be.
Then after quite some time, we were informed that life flight couldn’t travel with how the weather was. So, he was going to be taken to St. V’s by ambulance. We were told that with the amount of oxygen Brent was needing at the time, they wouldn’t have enough oxygen to get him all the way there. According to the medical records at 7 am his blood pressure was 124/79, pulse 106, and SpO2 92%. Someone with a SpO2 of 92% shouldn’t even be considered to be intubated, it’s not needed. It should also be noted that when he got there, he had a blood test done, and his blood glucose was almost 600. (He didn’t have a history of diabetes). Also, this hospital never tested Brent for Covid. When I asked about it, she stated that they take the patient’s word. (He was later tested at the other hospital and was positive). So, they wanted to start the Covid protocol without confirming if he had Covid or not.
While waiting for the ambulance to arrive a woman came into the room and stated that he needed to be intubated before they transport him or demanded he had to sign a DNR because they weren’t going to intubate him during the bumpy ride. We felt like we had no choice but to comply and let them put him on the ventilator. The thought of something happening to him on the way to the hospital that they were just going to let him die and not try to help him was terrifying. We trusted what the doctors recommended and at this point, we didn’t have a reason not to trust them. I always tried to avoid the news and any information on Covid in general, so I didn’t have much knowledge on how these hospitals were running things. Only if I knew then what I know now.
“During the 14 days that I wasn’t allowed to visit, I received ONE phone call from a doctor about my husband’s condition.”
I was in the room up until they were literally about to start the procedure which was around 10:15 am. I was not able to tell Brent a proper goodbye because there were at least 5 nurses around his bed at that time. It NEVER crossed my mind that, that would be the last time I ever got to see/talk to him while he was conscious. I truly believe that this hospital overreacted, over-treated, and over-medicated which caused a series of side effects and issues. They didn’t give him enough time on oxygen before they jumped the gun and intubated him. I do believe he did have diabetes and we didn’t know, and him having covid brought it to light and he was in diabetic ketoacidosis (DKA). Which can cause issues with breathing. He was later found to be in DKA after he was admitted to the other hospital.
After hours of not hearing anything, I called St. V’s to get an update. They informed me of what was going on. The first few days were ok, nurses were calling at least 3 times a day with an update on Brent. As the days went on the fewer calls I received. I was lucky to get one a day. I felt like I wasn’t in the loop on anything, and that nurses are not being forthcoming, or they are leaving things out. I never got notified right away about important things or his condition. To name a few, one day he had a 265/110 blood pressure for a period of 20-30 minutes per a nurse. At one point he had to have a blood transfusion, I was never notified. He also went into AFib and I had no clue about it. During the 14 days that I wasn’t allowed to visit, I received ONE phone call from a doctor about my husband’s condition, and most of it was talking about information on ECMO. I was told by a nurse that doctors should be calling daily. If it wasn’t for mychart, I would have known nothing!
Covid treatment-according to his medical records, he NEVER received Remdesivir (thank God)! On his records, it stated that Remdesivir was out the window. He got Decadron (Steroid) and Actemra (Tocilizumab) which can cause serious infections especially if you’re diabetic (which he did develop infections, along with blood clots). He was considered for ECMO, but they said that he was doing better. When in reality he wasn’t doing better they just didn’t want to give it to him. By the time he was declining he no longer was eligible to receive ECMO.
“I presented this paper to one of his doctors and he looked at it and said no, no, no.”
He was in the hospital for 14 days before I was able to visit him. I fought so hard to be able to get into that hospital. It is proven that having loved ones around them is beneficial in their recovery. Every nurse I talked to had a different answer as to when I could see him. After asking one nurse about when I could see him, he stated and I quote “He’s sedated, and paralyzed there isn’t much going on”. I’ve never been so disrespected in my life. I was beyond upset, hurt, insulted, and angry. I was told the infectious disease doctor is the one who ultimately decides so I asked several times for that doctor to call me. Of course, he never did. Although, my persistence paid off; they let him out of isolation three days early. I’ve never been so happy to see my husband. Now I could monitor everything they were doing and maybe get some real answers.
I did talk to one of his doctors that first day that I was there. He basically said they are doing everything that they can. I said there must be more treatment options. He said “Well we can do this one procedure called bronchoscopy which would clear out some mucus out of his lungs and be beneficial.” It’s sad that in the previous 14 days they never thought about doing this procedure. That I had to specifically ask for something else to be done. I did countless hours of research on different treatment options that have been used for Covid patients in electronic journals. I had a front and back page of treatment options that have been proven to be beneficial for patients. I presented this paper to one of his doctors and he looked at it and said no, no, no. He didn’t even look at the back page. He stated, “there are no more treatment options, they were just keeping him alive”. That he only has a 30% survival rate.
Everything that was wrong with him was because of what they were doing to him. He was on so many different medications for all different kinds of things. Every medication except what he was actually there for which according to them was Covid pneumonia. Also, one night I was talking to his night nurse, and she talked about how she was concerned about his sodium levels. I told her I felt like they were not giving him the correct treatment to get him better, and she agreed that they could be doing more. On another occasion, I asked a nurse about all the controlled substances that they were giving him and how it was going to affect his brain. The nurse had no clue how to answer that. I also brought up when he would be considered for a tracheotomy, and she responded that she hasn’t heard the doctors talk about it.
Since day one he was on Fentanyl, Propofol, Nimbex, Precedex, and Midazolam. He was on these drugs during the 19 days he was in the hospital. Did it take that many potent drugs to keep him comfortable? No wonder he had all these other issues going on. These drugs are deadly alone. Not to mention they all depress breathing. Especially given to someone like my husband that has never taken more than Tylenol.
“November 15th, 2021 wasn’t the day my husband was supposed to die.”
On day 19 the doctor decided that he was going to start proning him again. They did it in previous days but stopped because it no longer was helping. Three nurses came into my husband’s room to move him onto his belly. Well, it was discovered that he had a bowel movement and they needed to clean him up. His nurse asked me to step out of the room while they cleaned him up. I agreed to step out so I could go to the bathroom and make a phone call. Leaving that room was a huge mistake. Probably 10 minutes later someone called me from the hospital saying that I needed to get to his room because he was coding. When I got into his room, I couldn’t believe my eyes. There were at least 10 people in his room while they traded out giving my husband CPR. I stood at the end of his bed in complete shock. When they called his death, I asked what the hell happened. That he was fine when I was asked to leave the room. His nurse said that when they were turning him to clean him up that his ETT tube became dislodged.
He said that he got help right away, that there was a resident doctor in the hallway and a RT in a room nearby. (Which according to the medical records I received his story seems a little off compared to what others documented) While the RT was about to start bagging him, he asked the resident doctor to verify where the ETT tube was which was found to be in his esophagus. So, the resident doctor removed it and re-intubated him. (This is all noted in his records) I truly believe that these nurses were negligent and dislodged his breathing tube and tried to fix their mistake by trying to put it back in and letting precious seconds, minutes pass by before they got the help they needed. By the time he began getting oxygen it was too late, his heart gave out and he was gone. My husband is no longer here because these nurses compromised his airway and dislodged his breathing tube. His records that I have don’t cover hardly any of the minutes before his death but there is definitely mismanagement of his dislodged breathing tube and mismanagement of the code blue following.
November 15th, 2021 wasn’t the day my husband was supposed to die. His medical records from the day that he died showed his doctor reported that his Fi02 was 65%, and his SpO2 was 95%. His labs that day were ok, there were some results that were in a normal range or a little high or a little low. There was no indication that his organs were failing at this point. Also, during his 19 days of hell, no nurse or doctor ever told me that any of his organs were failing. Who knows if my husband would have pulled through and beat this horrible virus at the end of the day, but he wasn’t given a fair opportunity, his life ended in the hands of neglectful nurses and the hospital’s inhumane protocols.
I will fight for justice for my husband until I take my last breath. He didn’t deserve this nor did this need to happen. People need to be held accountable! My kids no longer have a father, I no longer have my soulmate. Our family is forever changed all over a dollar. This is happening to thousands of our loved ones, people need to wake up!! I pray no one has to go through this, the pain is indescribable. It’s happening to younger and younger individuals. The government and doctors only have one thing in mind and that’s a payday not to save lives. Covid is treatable, but it’s not in their protocol and they know their protocol is killing patients. I know this is hard to take in and believe but please do research before one of your loved ones ends up in the hospital fighting for their life!






















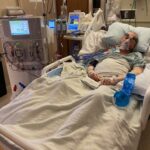










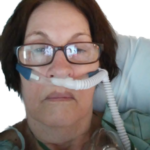














These are just a few of the cases archived by our COVID-19 Humanity Betrayal Memory Project, and there are more being reported by survivors and families of victims every day. If you would like to help with this project, please consider becoming part of the Task Citizens Force Against Instutional Capture And Crimes Against Humanity, a FormerFedsGroup Freedom Foundation mission.