I Have Chosen You To Live!





I have a letter I’ve been composing for the hospital, my latest version was written on 5/30/22. I’ve never managed to send it to them because I was trying not to be rude. My first attempt was written in March and I had to modify it because I was so emotional. It is the only hospital in our area and I was trying to find a way to tell them about my experience to help them improve — which was before I realized what they did was on purpose, as so many other hospitals. I really did not know this wasn’t an isolated occurrence. This letter is only for my 6-week hospital stay. I hope it gives you a view – even in a small way, of what I lived. I am happy to answer any questions. I have copied it in below – it gives details not just of what I endured on the Covid floor but even after they transferred me off the floor:
May 30, 2022
Dear UPMC
On December 4th, 2021, I came to the ER due to low oxygen saturation. I had been getting over bronchitis. But apparently it became pneumonia. Then while in the ER, an ER man stuck a huge q-tip up my nose – both nostrils – and tried to scoop out my brain. I tried to keep him from hurting me. He came back a short time later and pronounced it COVID….dnnnn, dnnnn, dnnnn (queue the scary music).
This began a six-week misery that I can say was not helped by UPMC “hospitalists”, but I get ahead of myself.
I am writing in the hopes I can point out areas where UPMC can improve their facility and treatment of patients. If you have no desire to do such things (as the local community believes – many call UPMC “the hospital of death”), you can ball up and toss away this letter. It will be a long letter, but I believe the information will be pertinent.
The ER:
My journey starts in the ER – which is run like a concentration camp or gulag. I was put in a room right across from an active ER desk , but the curtain was pulled across the glass wall in the room in which I resided. I spent two days in the ER, on an uncomfortable gurney bed in a freezing cold room. I was told there were “no beds”. I was give ONE blanket, oxygen, and a toilet chair against the wall next to the gurney bed. I was handed a call button. I must assume one of two things – either the Call Button did not work, or I was willfully ignored. I had to get up to use the toilet. On activity, my Oxygen Saturation dropped. I had trouble trying to get out of the bed. I pushed the button – no one came. I was freezing in that room. I pressed the button – no one came. I was thirsty and pressed the button – no one came. I was hungry and pressed the button – no one came —— shall I continue or do you get the picture? I begged a cleaner wiping the outside of the glass door to please get someone to bring me another blanket because I was freezing. The poor woman looked wide-eyed and horrified. Someone dropped off a blanket and disappeared. The second day I was practically thrown a tray of food I could not eat (I have dietary issues and allergies). The tray was placed on the floor by the glass wall – the one with the curtain enclosing me in the room like a shroud. My mother came to visit – she got me something to drink and more blankets. As new food was brought, each uneaten tray was dropped on the floor with the others in the corner. After three trays ended up on the floor in the corner, all I could think was, “There are going to be RATS in here”. My mother asked why I was still in the ER – we were again told there were “no beds”. No one cleaned the ER room I was in. By the time I left that room, the toilet chair was very full and stank. The food in the corner was equally disgusting. It seemed something you would see in a third world toilet of a hospital. So if you are saying UPMC is “great” – I really suggest you re-examine the ER practices.
Once I was eventually moved to a real bed in the hospital on the Covid floor, I was told they had beds and they didn’t understand why I was left in the ER for two days. So I ask, was it because I came in on a Saturday and no one wanted to bother? Either that or was the hospital staff waiting for me to die in the ER?
Now I ask the following out of curiosity – Do hospitals really get money for every Covid patient – and do you get a bonus when a person dies in the hospital of Covid? I would hope this is a vicious rumor because if true, don’t Hospitals become killing fields?Without care, many people who don’t come to the hospital will die – without care in the hospital, won’t they also die? I do not remember being given anything but oxygen in the ER, and food I could not eat due to dietary restrictions no one cared about. So – basically no care or minimal care when my mother insisted.
Any hospital more interested in profit than patients – that is inherently evil, is it not? Totally against the entire concept of patient care and patient rights, and an old important oath to”first do no harm”.
Suggestions for the ER:
The Covid floor:
I find it interesting that medicine is now thought to be all about “science”, when in fact it really isn’t. We must always factor in God. God is the great physician, the ultimate healer. To think otherwise is just human arrogance.
Once I was in an actual hospital bed, in a room that was moderate instead of freezing, I was more comfortable. However, the first “hospitalist” who came in asked me, with a long face, if I had “notified my family yet”. Nothing like telling a patient – you are going to DIE, tell your family. Is that really the kind of hospital you want to be known as – “the hospital of death”?
I told him I was in God’s hands. I would either be healed or go home to my Lord in heaven – a win-win with no downside. He was shocked and did not know how to respond.
As for the Covid floor – I feel bad for the nurses. I suggest that in future when a patient is transferred off the Covid floor because they are doing better – that you post that for all the nurses to see — so they don’t think every patient that disappears died. One nurse eventually was assigned to the floor I was transferred to and she was so thrilled to see I was still alive.
The Covid floor does not have to be a place of death. Nor should it be miserable for the nurses working there. It is just another disease. Deadly in some cases. But so is every other disease – deadly in some cases.
Remember, we should not be so afraid to die that we stop living. Only God knows the day, time and manner of our death.
Hospitalists:
What I experienced under the “hospitalists” was nothing short of experimentation. In my opinion, it was not medicine. It was whatever the latest “hospitalist” wanted to try. It was really horrific. The “hospitalists” changed every 3-5 days I believe. There was always a new one. And each one did something different – sometimes seeming to wipe out the orders of the previous one and starting something new.
As I look back, I can honestly say I question the credentials of every so-called “hospitalist”. I now want to see a resume, diplomas, references from where they have worked and patients they’ve treated who lived, and numbers on how many died under their care.
What UPMC is doing wrong – NO COORDINATED PATIENT TREATMENT PLAN. It is a crap shoot – or that is what it looked like to me and my 80 year old mother. Mom has had over 35 surgeries in her life – she has been in a lot of hospitals. I believe she told off several hospitalists while I was in there.
What did I endure?
Hospitalists who refused to give me all the prescribed maintenance medications I take every day. Only some of them were allowed. Also – NONE of my daily supplements were allowed even the ones I was told to take by my doctors. Two examples – magnesium, and gentle iron — so when bloodwork came back saying I was deficient in these – gee, ya think?!!! If you will not honor the meds and supplements people take every day – then let the patient have the meds and supplements brought in and administered by the patient or family caregiver.
Hospitalists who refused to give me any therapeutic, such as Ivermectin. Who kept insisting they had to follow the “approved mandated hospital protocols”.
Hospitalists who refused to listen when I said I was NOT diabetic, never have been. My fingers were 6 weeks of pincushions from multiple glucose tests every single day.
A hospitalist who decided I needed a “PICC line” and intravenous feeding. I went 5 days without anything but a glucose IV while they figured out what they were going to create in the lab to inject into me. I was starving, begging for food! I did lose over 20 pounds in a six week period at UPMC. I do not recommend it. It was not healthy. It made me weaker.
A hospitalist who decided I needed to be on complete bed rest – no more toilet chairs for me because my oxygen saturation went down when I got up to go and then get back into bed. They would NOT listen to me that I had it worked out to rest on each movement and get my oxygen saturation back up again before I did the next movement. Why was this STUPID on the part of the hospitalist? Because my oxygen saturation STILL goes down on movement and exertion and I’m HOME now and living on supplemental oxygen. But as a result of this TERRIBLE directive, I lost the ability to stand, walk, get up from a seated position, go to the bathroom on my own, shower, and otherwise move around under my own power. I also ended up with bad spots (sores) on my behind from laying in my own urine and feces when the few “bad” nursing assistants, who did not bring bed pans quickly, then ignored my need to be cleaned up and left me laying in bed for hours until someone took pity on me and cleaned me and changed my bedding.
Hospitalists – plural – who kept trying to put me on a ventilator. And who kept pushing the ventilator and mentioning remdesivir. For Covid, a ventilator is DEATH – everyone knows that. I refused. My mom (who is power of attorney and ADR representative) also adamantly refused. I’m still alive – so guess what – we were right and the hospitalists were WRONG.
A hospitalist who said I needed a BiPAP. And I tried that for a few days (5 days I think)- however, they could not get all my meds intravenous and they had me shoving pills in the side of the mask into my mouth then using a straw shoved under the mask to take water to wash down the pills. I later learned this was VERY DANGEROUS – as in trying to kill me – because this could have caused water in my lungs and even worse illness if not death. Again I ask, was UPMC trying to kill me? I demanded to be taken off after about 5 days, was warned it was “dangerous”, but I insisted they try be back on regular oxygen instead. And I was fine WITHOUT the BiPAP. So I ask now, did I ever really need it? I now doubt that I did. And I believe if I had stayed on it, it would have further injured my lungs.
Hospitalists who gave me so much steroids that I went from no cataracts to needing cataract surgery this year. I just turned 60 in January. I saw my eye doctor for my yearly eye exam in May. They were shocked and wanted to know how this happened. It was the only explanation they could come up with, the steroids given at the hospital caused cataracts to form that are “ripe”. This may have been necessary, but it would have been nice to be warned about it.
Hospitalist who was a nice man but did not understand that if my nostrils were clogged with blood clots, the cannula just wouldn’t work to give me oxygen. If you can’t inhale through your nose, it just won’t work. When I had an anxiety attack because I couldn’t breathe and he came in during that, the poor man fell apart and could not help me and was desperate to get a nurse so he could leave. And THAT is why I question the credentials of these “hospitalists”. That was NOT the response of a real doctor when he comes in to find a patient gasping and having trouble breathing, and he runs out the door to get a nurse! I was denied both an ENT and Pulmonologist doctor visit.
The final hospitalist was the worst I think. She came in my room and for reasons I will never understand, as I’d never met the woman before, she took a dislike of me. She tried to restart the blood thinners I’d been taken off of for several days. I had terrible nose bleeds due to the oxygen. I was grateful when I was taken off the blood thinners. With no explanation – especially when a chest CT showed NO blood clots whatsoever, this hospitalist put in an order to give me blood thinners. When the nurse brought it in, I asked what it was, she told me, and I REFUSED. I was finally able to breathe through the cannula as some of the debris had cleared from my sinuses. That hospitalist really didn’t like me. She tried to transfer me to a nursing home with inferior rehab and care (that is part of UPMC) – not the one I’d requested and whom had said I had a bed. Allegany Health Nursing and Rehabilitation (they have an excellent rehab center) had worked it out already, but we needed to get through the MLK holiday weekend. This hospitalist decided she would lie to me about Allegany Health NOT having a bed for me – a verifiable lie. Then she lied and told me I was being transferred to where I wanted to go. It was only in the afternoon of the 17th of January that the nurse told me the name of where they were transferring me, and I learned the hospitalist had lied to me. I was in tears. I refused. I called my mother. She appealed this decision. Bright and early January 18th, once Allegany Health opened up, I was told I was transferring there at 2:30pm that day (which happened to be my birthday). God gave me a wonderful birthday gift. However, that hospitalist came to my room one last time to sneer at me and say, “I see you got to go where you wanted after all.” Please explain to me WHY where I went for rehab mattered to a woman I had never met and never seen prior to that weekend when she came to my hospital room. Why did she care? Why did she dislike me? Or was she operating under UPMC orders?
These are only some examples. Not having real doctors, and you will never convince me these hospitalists are “real” doctors with United States degrees, residency, and licensing. (Not transferred or experience from another country stuff), not having real doctors is a detriment to patient care. It may be great for your profit margin, but it is NOT great for patients. A primary care doctor knows the patient, their history, their meds. They can talk to a hospital doctor in doctor speak, work out a real plan of care. A “hospitalist” who switches out ever few days – do they care about the patient AT ALL – the answer is – probably not. In that case, it’s a job, not a calling to heal.
Stop thinking of UPMC “profits” and go back to thinking of “patients” and their care and healing. To think of profits is to invite disaster and operate under an inherently evil agenda. Money is NOT everything. Love of money is the root of all evil.
Nursing staff:
The nursing staff on the other hand is 99.98% fabulous. There were only a couple that were awful and they were young assistants usually on graveyard shift who didn’t want to be bothered by patients who needed something. The rest were just great and awesome. I loved the majority of the nurses and nurse assistants.
I believe the worst part of the problem is lack of staff. I was not kept clean or given the means of keeping myself clean. My mother helped when she was there each day and that is how I survived my stay. It was horrible to feel dirty all the time. I learned quickly there is no place for modesty in a hospital bed when you are on bedrest and too weak. I was stripped naked and not covered while men and women entered the room. It was the only way to get clean once someone was actually willing to clean up the human waste mess in my bed, or the times I was given a spit-bath, which was NOT daily.
I’d say the worst assistants were on the graveyard shift, as detailed earlier in this letter. Nothing like leaving a patient to sit in their own waste for hours. That happened a few times, until a wonderful nurse came in one morning and started to clean me up after I told her no one had come yet and I was messy. When her assistant (who had come in the day before and cleaned me up after shift change) told the nurse this was the same way she found me the day before, the nurse said this was “unacceptable”. I must admit, I think someone got fired or reassigned over that one because it didn’t happen again.
I loved the nurses and nursing assistants – both on the Covid floor and the floor I got moved to. One nurse, Maria, was working another section, but she came to help me when my mom asked her to get someone to help me. Maria was the only one mom found, and Maria came and she was wonderful. She is an example of the excellent nursing staff.
I feel the non-nursing staff need more training. If I press the “help” button, don’t ask me to explain what I need over an intercom, and don’t ignore me if you hear no voice response. And don’t get angry with my lack of audible response. Do you know how hard it is to say a word when you are on 15 liters of oxygen and gasping for air? The staff doesn’t understand that the intercom doesn’t work for all patients, and pressing that button IS asking for help, not necessarily just asking for ice water – sometimes it is a life threatening situation and the patient cannot respond. Is taking off my oxygen mask so a staff member can hear me over the intercom really the best plan? Taking the time to ask for details over an intercom seems life-threatening in itself, depending on the patient. At one point, my monitoring devices were sounding an alarm and no one came for a VERY long time. I pressed the button and NO ONE CAME. I tried to yell for help, and NO ONE CAME. What if that was your loved one pressing that button? When you are confined to bed rest – all a patient can do is press that button and pray someone comes.
Physical therapy
Once I was moved off the Covid floor, I was put in another room and we were trying to get my oxygen liters down. They also decided it was time for physical therapy since I’d been on bed rest for weeks. Only problem is – when they came, there was a shrill woman I believe was in charge of physical therapy (PT) who was ordering everyone around. They did not really explain what I needed to do, what to expect. I was having anxiety attacks, and when I couldn’t do what they wanted due to muscle weakness, I was told it was my fault, that I could do it if I just tried. But I was trying, and failing, and crying in frustration and fear.
UPMC PT didn’t use a belt on me that I remember. They pulled on my arms (and I have a torn rotator cuff on the left side). It was painful. One time, they sent a tiny girl – by herself – who told me she could hold me and catch me and lift me. The girl had toothpick arms. I out-weighed her, by a lot, even having lost about 25 pounds by that point. Sheer physics dictated that if I started to topple, I would take her with me. Period. I did not want to fall and injure myself, or her.
Another time they sent me a PT tech who was like 8 months pregnant. I am NOT going to be responsible for injuring an unborn baby.
Some of the PT techs were nice. I did not like the shrill woman who made me feel like such a failure, and she came most often. Though they really didn’t come by a lot, now that I think about it. I’m not sure why. I know I was really exhausted and my muscles just wouldn’t hold me. When I was constipated, I was in a lot of pain. But mostly I battled fatigue – I’m still battling it. My anxiety attacks were really bad. My body would not cooperate. And I really didn’t know what everyone wanted from me. I knew I needed to relearn how to walk and stand up, but I could not get my muscles to cooperate. I required the oxygen, and on activity my ox sat went down low. I had no strength, and instead of strengthening my muscles, the PT lady was trying to get me to do all the things my muscles could not do, with no real understandable plan that I could grasp. She even took me off the monitor and was not respectful of my fear. So I failed, was embarrassed, was terribly afraid I would never be able to walk again. It was a cycle that just spiraled into a pit. All because of the way I was treated by the shrill woman.
How do I know it was a problem particular to UPMC? Because of what happened at Allegany Health Nursing and Rehabilitation. It was night and day. They made sure I felt secure, with a sturdy PT belt that had loops – no one pulling on my arms. They were positive and celebrated every little thing I was able to do. They started me on exercises for my arms and legs to strengthen them – and these were the things I did each day Mon-Fri. The first day of therapy they put on the belt and had me walk a few steps, but I got tired real fast and had to sit down. NO ONE said I didn’t do enough. They told me what I did was great. Even when I apologized for not doing more, they said that was why they were there, to help me get back on my feet. The way they did PT and Occupational Therapy were positive reinforcement and celebration – no nagging, no negativity, no shrillness. And they didn’t try to take away my oxygen and scare me to death. They kept a monitor of my ox sat level, and had me rest and breathe as needed.
Suggestion for PT:
Get training and learn what positive reinforcement is about, and don’t make a person feel bad for what they can’t do. And do not decry a person’s fears but work around them. Support the person so the person gains confidence, and if that patient is using something as a crutch, even if it is a stuffed bear they need to hold – let them until they gain the confidence and put the stuffed bear down because they don’t need it anymore. People who have lost the ability to walk because of bed rest for weeks – treat them with respect but like children emotionally – in constant need of encouragement and genuine caring. It isn’t something you can fake – do you not know when someone is faking how they feel about you? Some people respond to harsh and military orders, others crumple. Find what works best for each person. Adjust the plan for the patient.
General suggestion:
Invest and get better wi-fi reception and boosted cellular signals in the hospital rooms. There has to be a way to do this without causing issues. Not being able to use a cell phone or tablet to get online was just awful. It would be nice to watch a movie, or get well-wishing texts. Being isolated and alone for weeks without end at a hospital is a horrible thing.
I really hope you review what I’ve written and take it to heart. You are the hospital we have. It would be nice if you changed your attitudes and actions so no one calls you “the hospital of death” anymore. I would love to see the surrounding community start saying what a loving and nurturing hospital, such excellent staff in all areas, such excellent care, etc. And I would hope you would not use my honesty against me, or retaliate against me, should I ever find myself in need of emergency care, or extended care, or surgeries in future.
Please note I sent a separate letter on the UPMC Western Maryland Home Care that I received after leaving the nursing home rehab center. The Home Care was AWESOME.
Thank you for your time.
Sincerely yours,
Dana Hites









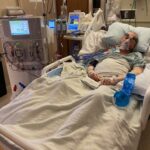







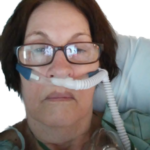






























These are just a few of the cases archived by our COVID-19 Humanity Betrayal Memory Project, and there are more being reported by survivors and families of victims every day. If you would like to help with this project, please consider becoming part of the Task Citizens Force Against Instutional Capture And Crimes Against Humanity, a FormerFedsGroup Freedom Foundation mission.